“The true measure of a robust revenue cycle isn’t how many claims you submit, but how few you have to fight for.” – [Cite Moz 2024 here]
The $5 Million Leak: Why Your Revenue Cycle is Secretly Bleeding Cash
The healthcare industry operates on thin margins, yet many providers unknowingly leave millions on the table. The average facility sees up to 10% of its total revenue lost due to preventable claim rejections, turning potential profit into frustrating administrative overhead. This leakage is symptomatic of weak Claim Denial Management practices that fail to identify and address systemic failures.
This isn’t just about chasing rejected money; it’s about fixing the foundation of your financial health. We’re moving beyond reactive appeals and toward proactive defense, focusing on techniques that maximize your First-Pass Acceptance Rate immediately. The goal is to transform your financial team from claim fighters into revenue cycle architects.
- Denials inflate Accounts Receivable Days (A/R), tying up capital.
- They divert staff time away from higher-value patient care tasks.
- Chronic denials signal deep-seated problems in your coding and documentation.
The Harsh Truth: What Top Payers Say About Claim Denial Root Causes
To master Claim Denial Management, you must first identify the true source of the pain. Most denied claims stem from a handful of repeatable, predictable errors that can be traced back to the registration and documentation phases. A systematic Root Cause Analysis reveals that these issues are rarely one-offs.
Decoding the Denial: Eligibility, Prior Auth, and the Gatekeepers
A shocking number of rejections occur before a service is even rendered. Insufficient or inaccurate Patient Eligibility Verification is a common culprit, leading to immediate non-payment. Similarly, failing to secure necessary Prior Authorization Issues turns a billable service into a financial write-off.
Payers are strict gatekeepers, and missing these administrative steps is viewed as a clear breach of protocol. Your front-end staff needs streamlined processes and real-time tools to combat these preventable errors effectively. Ensuring correct patient data before the encounter starts is the first line of defense.
- Verify coverage details and benefit limits meticulously.
- Track and document all authorization numbers in the patient record.
- Train staff to recognize high-risk services requiring pre-approval.
The 3-Pillar Framework for Proactive Claim Denial Management
High-performance organizations shift their focus from recovering denied funds to preventing the denial in the first place. This requires a structural overhaul of your Claim Denial Management Process Flow, built on three interlocking pillars designed for maximum efficiency.
Pillar 1: Stop Errors Before Submission with Claims Scrubbing
The single most impactful step in boosting your First-Pass Acceptance Rate is implementing robust Claims Scrubbing software. This technology acts as a powerful internal auditor, checking claims against thousands of payer rules before they leave your facility. This prevents errors like unbundling or missing modifiers.
- Claims Scrubbing systems use payer-specific logic.
- They verify data consistency between the clinical and billing systems.
- Immediate feedback loops train your billers and coders.
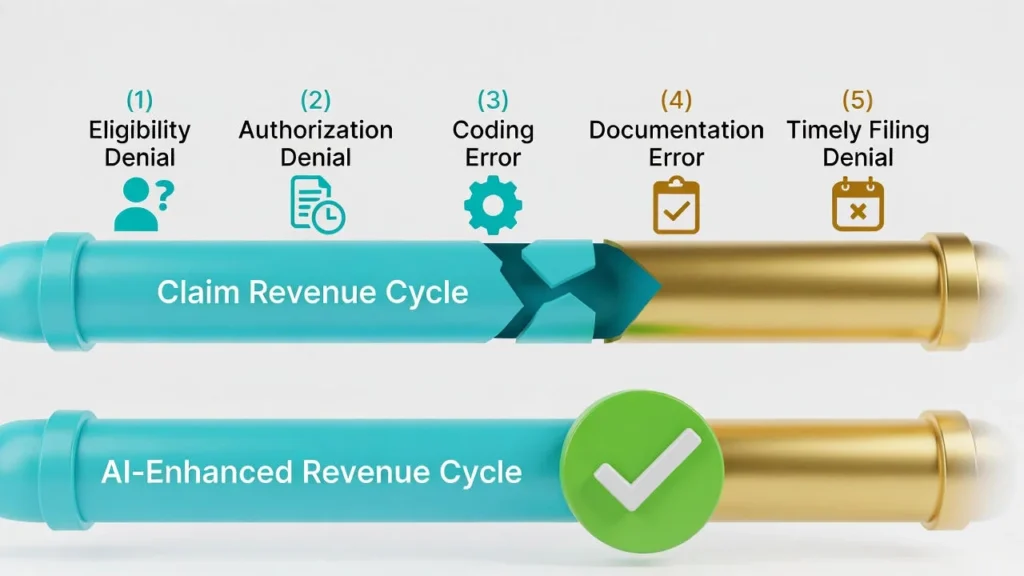
Pillar 2: Master the Art of Medical Necessity Documentation
To beat a Medical Necessity Denial, your clinical records must speak a unified language that payers understand. Clinical Documentation Improvement (CDI) programs ensure that the patient’s acuity, complexity, and treatment journey are clearly reflected in the notes. This is where your providers’ expertise is converted into billable revenue.
If a payer suspects the service wasn’t medically necessary, no amount of appeals paperwork will fix thin documentation. The key is embedding documentation best practices directly into the provider workflow using your EHR.
Pillar 3: Close the Gaps in Payer-Provider Communication
Many delays and denials are caused by simple misunderstandings or lack of information exchange during the claim lifecycle. Establishing clear lines of Payer-Provider Communication is critical, especially when dealing with complex cases or navigating changing policies.
Utilize direct electronic connections and payer portals to quickly verify benefits, confirm authorizations, and check claim status. This reduces the friction that leads to Coordination of Benefits (COB) headaches and delays.
Case Study: How a Small Practice Recovered 92% of Denied Claims
A small multi-specialty clinic faced a recurring 15% denial rate, leading to six-figure monthly losses. After implementing a strong Denial Prevention Strategy, they focused on Root Cause Analysis and identified prior authorization and eligibility as the primary culprits. They retrained front-office staff and integrated a real-time eligibility checker.
Within six months, their denial rate dropped to 3%. More importantly, their Lost Revenue Recovery rate jumped from 60% to 92% because the few remaining denials were high-quality, easily appealable claims. This success story proves that process discipline is the ultimate competitive advantage.
Beyond Billing: Using AI and Data to Supercharge Your Claim Denial Strategy
The future of Claim Denial Management lies in leveraging technology to stop fighting history and start predicting the future. This is where advanced tools elevate the role of your billing staff.
The Crystal Ball: Predictive Denial Analytics in Action
Modern Practice Management (PM) Software utilizes Predictive Denial Analytics to assign risk scores to claims before they are submitted. By analyzing historical denial patterns, the system highlights which claims are most likely to be rejected.
This proactive data science allows your team to intervene only where it matters most, leading to hyper-efficient workflows. You can monitor high-risk trends in a Denial Log Tracking system, which gives you real-time intelligence on payer behavior.
- Flag claims with high historical error rates for review.
- Identify specific payer/procedure code combinations that are high-risk.
- Use data to justify investments in Clinical Documentation Improvement (CDI).
Automating the Fight: RPA for Appeals and Resubmission
For the few claims that still require an appeal, Robotic Process Automation (RPA) is a game-changer. RPA bots can handle the time-consuming, repetitive steps of preparing the Claims Resubmission packet, accessing payer portals, and uploading supporting documents. This frees up human billers for complex, high-value appeals.
Integrating Your Tech: EHR, PM, and the Seamless Workflow
True efficiency in revenue cycle management demands that all systems talk to one another. Electronic Health Record (EHR) Integration with your PM and billing systems eliminates manual data entry and reduces the risk of Incomplete Documentation. A seamless workflow, leveraging Denial Management Best Practices, ensures that clinical data automatically flows to the billing side, minimizing transcription errors and improving claim quality.
The Final Battle: Creating an Ironclad Claims Denial Appeals Checklist
When a claim denial hits, your response must be immediate, organized, and strategic. Having an Appeals Checklist ensures your team does not miss any critical steps.
Step-by-Step: The Ultimate Appeals Preparation Workflow
The key is to conduct a thorough review to determine if the claim is appealable or simply needs a minor correction and Claims Resubmission.
- Verify the reason code against the patient file.
- Gather all supporting documentation (including clinical notes and authorizations).
- Draft a clear, concise appeal letter citing the payer’s own policies.

The Clock is Ticking: Why You Must Cut Your Accounts Receivable Days
Every day a claim sits unpaid, your facility is losing money. Effective Claim Denial Appeals must be filed swiftly to adhere to strict payer deadlines and move the outstanding balance. Reducing your Accounts Receivable Days (A/R) is the ultimate metric for successful Claim Denial Management.
“Mastering claim denials is not an administrative burden; it is the single greatest lever you have to control your financial destiny.”
