Understanding CPT vs ICD-10 is fundamental to accurate medical coding and successful claim reimbursement. While both coding systems are essential in healthcare billing, they serve distinctly different purposes—and knowing when and how to use each can mean the difference between clean claims and costly denials. Medical coders, billing specialists, and practice administrators must master both code sets to ensure proper documentation, maintain coding compliance, and optimize revenue cycle management. This comprehensive guide breaks down everything you need to know about CPT codes and ICD-10 codes, their relationship in the billing process, and best practices for coding accuracy.
Whether you’re new to medical coding basics or looking to refine your procedural coding and diagnostic coding skills, this guide will help you navigate these critical healthcare coding systems with confidence.

What Are CPT Codes? (Understanding Procedural Coding)
CPT codes, or Current Procedural Terminology codes, are the standardized numerical codes used to describe medical, surgical, and diagnostic services performed by healthcare providers. Developed and maintained by the American Medical Association (AMA), CPT codes document what procedure or service was performed during a patient encounter. These five-digit codes are essential for healthcare claims submission and insurance billing.
The CPT coding system provides a uniform language that describes medical procedures and services. When a physician performs an office visit, conducts a surgical procedure, or orders a diagnostic test, the appropriate CPT code captures that service for billing purposes. This standardization ensures that payers understand exactly what services were rendered, facilitating accurate reimbursement.
CPT Code Categories Explained
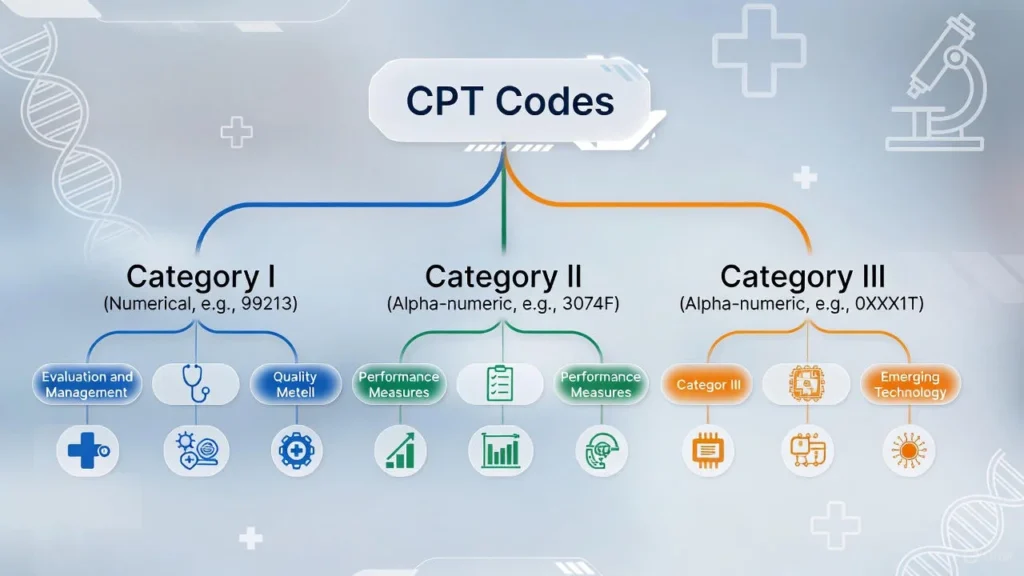
CPT codes are organized into three distinct categories, each serving specific documentation needs:
Category I CPT Codes are the most commonly used codes in medical billing. These five-digit numerical codes (ranging from 00100-99499) describe widely performed procedures and services. Examples include 99213 for an established patient office visit or 45378 for a diagnostic colonoscopy. Category I codes are updated annually and represent procedures with proven clinical efficacy.
Category II CPT Codes are supplemental tracking codes used for performance measurement. These four-digit codes followed by the letter “F” (like 3074F) help measure healthcare quality and aren’t typically used for reimbursement. They track specific clinical outcomes and quality metrics for reporting purposes.
Category III CPT Codes are temporary codes for emerging technologies and procedures. These codes (like 0XXX1T) allow data collection for new services before they receive permanent Category I status. They’re crucial for innovation in healthcare coding system development.
How CPT Codes Are Structured
The CPT structure follows a logical five-digit format that groups similar services together. The first digit often indicates the general category, while subsequent digits provide increasing specificity. For instance, codes beginning with “9” typically relate to evaluation and management services, while “7” codes often indicate radiology procedures.
CPT modifiers add another layer of detail to procedural coding. These two-digit codes (like -25 or -59) attach to CPT codes to provide additional information about the service performed. A modifier might indicate that a procedure was performed on multiple sites, by multiple physicians, or under unusual circumstances. Understanding CPT modifiers is crucial for accurate medical billing accuracy and avoiding claim denials.
Common CPT Code Examples in Practice
Let’s examine real-world CPT code applications. Code 99213 represents a level 3 established patient office visit requiring moderate medical decision-making. Code 93000 describes a complete electrocardiogram with interpretation. Code 80053 identifies a comprehensive metabolic panel, a common laboratory test.
These codes appear on every claim form alongside their corresponding charges. The specificity of CPT categories ensures that different complexity levels and service variations receive appropriate reimbursement. A simple office visit (99212) carries a different value than a complex visit (99215), reflecting the time and clinical expertise required.
What Are ICD-10 Codes? (Understanding Diagnostic Coding)
ICD-10 codes, or International Classification of Diseases, 10th Revision, represent the global standard for diagnostic coding. These codes document why a service was performed—the patient’s diagnosis, symptoms, or health condition that justified the medical intervention. Maintained by the World Health Organization (WHO) and adapted for U.S. use by the Centers for Disease Control and Prevention (CDC), ICD-10 codes are essential for healthcare documentation and medical necessity justification.
Unlike CPT codes that describe what was done, ICD-10 codes explain why it was necessary. When a provider orders a chest X-ray (CPT 71046), the ICD-10 code might be J18.9 for pneumonia, unspecified, establishing medical necessity for the procedure. This diagnostic information is critical for payer rules compliance and successful reimbursement.
ICD-10-CM vs ICD-10-PCS: Key Differences
The U.S. uses two versions of ICD-10 coding: ICD-10-CM (Clinical Modification) and ICD-10-PCS (Procedure Coding System). Understanding this distinction is vital for proper code selection.
ICD-10-CM codes are used by physicians, clinics, and outpatient facilities to report diagnoses and reasons for healthcare encounters. These alphanumeric codes range from 3 to 7 characters and begin with a letter. For example, E11.9 represents Type 2 diabetes mellitus without complications. Most medical billing professionals work primarily with ICD-10-CM codes for claim submission.
ICD-10-PCS codes are used exclusively by hospitals for inpatient procedure coding. These seven-character alphanumeric codes are far more specific than CPT codes and apply only to hospital inpatient settings. Outpatient facilities and physician practices use CPT codes for procedures, not ICD-10-PCS.
ICD-10 Code Structure and Format
ICD-10-CM codes follow a hierarchical structure that increases in specificity from left to right. The first three characters represent the category of disease or condition. Characters four through six provide increasing clinical detail about anatomical site, severity, or other specificity. The seventh character, when required, adds information about episode of care or laterality.
For instance, code S82.001A breaks down as follows: S82 indicates fracture of the patella, .001 specifies unspecified fracture of right patella, and A indicates initial encounter for closed fracture. This granular detail supports accurate healthcare documentation and provider documentation requirements.
The specificity requirements in ICD-10 coding are significantly more detailed than the previous ICD-9 system. With over 70,000 available codes, ICD-10 allows precise documentation of patient conditions, complications, and treatment circumstances. This specificity improves data quality for clinical research, public health tracking, and insurance billing accuracy.
Real-World ICD-10 Coding Examples
Consider these common diagnostic codes in practice. Code I10 represents essential (primary) hypertension, one of the most frequently used diagnostic codes. Code Z00.00 indicates an encounter for general adult medical examination without abnormal findings. Code M79.3 describes panniculitis, unspecified, addressing soft tissue inflammation.
More complex scenarios require multiple ICD-10 codes. A patient presenting with chest pain (R07.9) might receive additional codes for coronary atherosclerosis (I25.10) and nicotine dependence (F17.210), painting a complete clinical picture. This comprehensive diagnostic documentation supports the CPT and ICD relationship necessary for medical necessity validation.
CPT vs ICD-10: The Key Differences
The fundamental distinction in CPT vs ICD-10 lies in their purpose within the healthcare billing cycle. CPT codes answer “what was done” while ICD-10 codes answer “why was it done.” These complementary code sets work together to tell the complete story of a patient encounter, but they serve entirely different functions in medical coding and billing.
Understanding these differences is essential for coding accuracy, compliance with coding guidelines, and preventing billing audits. Let’s examine the critical distinctions between these two coding systems.
Purpose: Procedures vs Diagnoses
CPT codes document procedures, services, and treatments provided to patients. They capture physician work, facility resources used, and the complexity of services rendered. When a cardiologist performs an echocardiogram, a CPT code identifies that specific diagnostic procedure.
ICD-10 codes, conversely, identify the patient’s medical condition or the reason for seeking care. They establish medical necessity by documenting symptoms, diagnoses, injuries, or health status. The ICD-10 code explains why the echocardiogram was medically appropriate—perhaps due to heart failure (I50.9) or chest pain (R07.9).
Code Ownership and Updates
The ownership and maintenance of CPT vs ICD-10 codes differ significantly, affecting how updates are implemented and who governs coding changes.
CPT codes are proprietary codes owned and copyrighted by the American Medical Association. The AMA’s CPT Editorial Panel updates these codes annually, typically implementing changes each January. New medical procedures and technologies drive most additions, while obsolete codes are deleted. Healthcare providers must purchase current CPT code books or subscribe to coding software to access official codes.
ICD-10 codes are maintained by the World Health Organization internationally, with the U.S. version (ICD-10-CM) adapted by the CDC and CMS. ICD-10 updates 2025 and annual revisions occur on October 1st each year, aligning with the federal fiscal year. These updates reflect new diseases, refined clinical knowledge, and improved specificity requirements. Unlike CPT codes, ICD-10 codes are publicly available without licensing fees.
Usage in Medical Documentation
In practice, CPT vs ICD-10 codes serve different documentation functions within EHR systems and medical records. CPT codes typically appear on charge tickets, superbills, and procedure documentation. They link directly to fee schedules and reimbursement rates, making them central to revenue cycle management.
ICD-10 codes integrate throughout the medical record, from the problem list to progress notes and discharge summaries. They support clinical decision-making, track patient health over time, and justify the medical necessity of ordered services. Quality reporting, risk adjustment, and population health management all rely heavily on ICD-10 diagnostic data.
How CPT and ICD-10 Work Together in Medical Billing
While CPT vs ICD-10 codes serve different purposes, they must work in harmony for successful healthcare claims processing. Every medical claim requires both code types, creating a complete narrative of patient care that satisfies payer requirements and justifies reimbursement. Understanding this interplay is crucial for clean claims and efficient RCM workflow.
The coordination between procedural and diagnostic coding represents one of the most critical aspects of accurate medical billing. When these codes align properly, claims process smoothly. When they don’t, denials and payment delays follow.
The CPT and ICD Relationship in Claim Submission
Think of a medical claim as telling a story: the diagnosis provides the “why” and the procedure provides the “what.” Together, they demonstrate that the services rendered were medically appropriate and necessary. This is the essence of the CPT and ICD relationship.
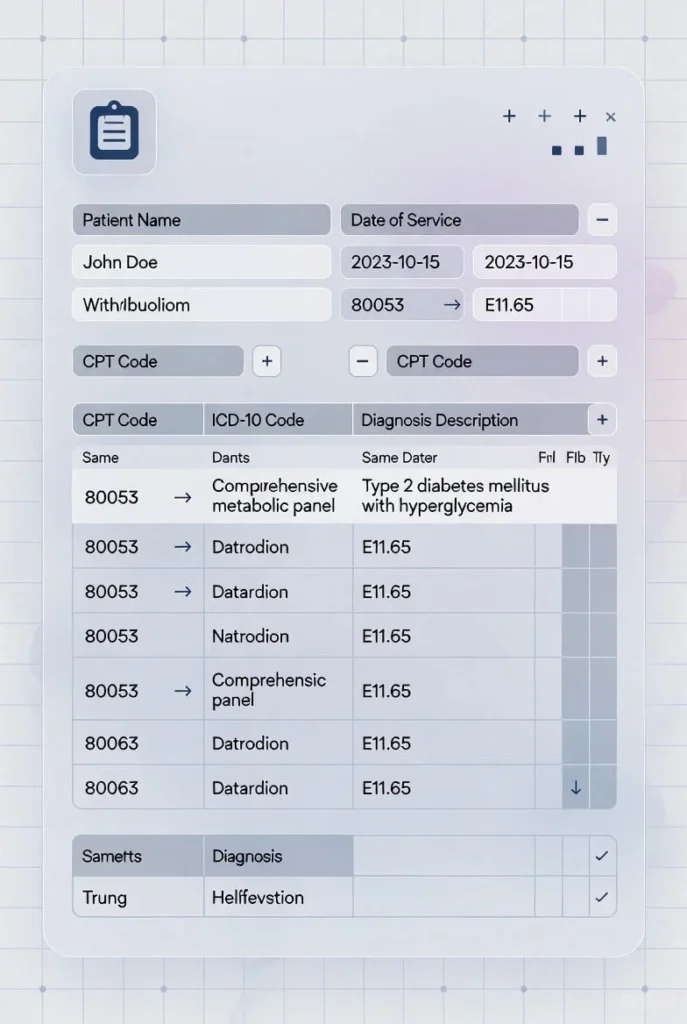
For example, if a provider performs a comprehensive metabolic panel (CPT 80053), the claim must include a diagnosis that justifies this laboratory test. Acceptable ICD-10 codes might include E11.65 (Type 2 diabetes with hyperglycemia) or N18.3 (chronic kidney disease, stage 3). The diagnosis proves the test was medically indicated, not performed randomly or unnecessarily.
Why Both Codes Are Required for Reimbursement
Insurance companies and government payers like Medicare require both CPT vs ICD-10 codes for several critical reasons. First, they need to verify medical necessity—proving the service was appropriate for the patient’s condition. Without a valid diagnosis, payers cannot determine whether the procedure should be covered under the patient’s benefits.
Secondly, code pairing enables accurate claims processing and payment determination. Different diagnoses may affect reimbursement rates for the same procedure. A screening colonoscopy (CPT 45378) with diagnosis Z12.11 (encounter for screening for malignant neoplasm of colon) may process differently than a diagnostic colonoscopy with diagnosis K92.1 (melena/blood in stool).
Medical Necessity and Code Pairing
Medical necessity is the cornerstone principle linking CPT vs ICD-10 codes. This concept determines whether a service is reasonable and necessary for diagnosing or treating a patient’s condition. Payer rules define medical necessity through coverage policies that specify which diagnoses support which procedures.
For instance, a vitamin D test (CPT 82306) requires a diagnosis suggesting deficiency risk—perhaps osteoporosis (M81.0) or chronic kidney disease (N18.9). A routine annual exam diagnosis (Z00.00) would not typically support this test, potentially resulting in denial. Medical coders must understand these coverage requirements when assigning codes.
Common Mistakes When Using CPT vs ICD-10 Codes
Even experienced medical coders make errors when working with CPT and ICD-10 codes. These mistakes cost healthcare organizations millions in denied claims, delayed reimbursement, and compliance penalties. Understanding common pitfalls helps practices implement better coding best practices and improve their healthcare billing outcomes.
Avoiding these frequent errors requires ongoing education, attention to detail, and systematic quality checks throughout the coding and billing process. Let’s examine the most problematic areas where coding mistakes occur.
Incorrect Code Pairing Leading to Denials
The most frequent coding error involves submitting CPT vs ICD-10 codes that don’t logically connect. This mismatch confuses payers and triggers automatic denials. For example, pairing a mammogram (CPT 77067) with a diagnosis of foot pain (M79.671) lacks medical logic and will be rejected.
Another common pairing error occurs when coders select non-specific diagnosis codes that don’t sufficiently justify the procedure’s complexity. Using “unspecified” codes when more specific options exist can result in denials or downcoded payments. If documentation supports it, E11.65 (Type 2 diabetes with hyperglycemia) is preferable to E11.9 (Type 2 diabetes without complications).
Using Outdated Codes (ICD-10 Updates 2025 and CPT Updates)
Medical codes change annually, yet many practices continue using deleted or revised codes from previous years. This happens when coding software isn’t updated promptly, when coders rely on old reference materials, or when practices don’t invest in continuing education.
CPT codes typically update each January, with the AMA announcing changes several months in advance. New codes reflect emerging procedures and technologies, while obsolete codes are deleted. Using a deleted CPT code results in immediate claim rejection, as payers’ systems won’t recognize invalid codes.
Upcoding and Compliance Issues
Upcoding—selecting higher-level codes than documentation supports—represents a serious compliance violation. This might involve choosing a more complex office visit code (99215) when documentation only supports a moderate visit (99214), or selecting a more extensive procedure code than actually performed.
While sometimes unintentional, upcoding attracts scrutiny from payers and government regulators. The Office of Inspector General (OIG) actively monitors billing patterns for upcoding indicators. Practices that consistently bill higher-level codes than peers face increased audit risk and potential fraud allegations.
Best Practices for CPT and ICD-10 Coding Accuracy
Achieving consistent coding accuracy requires systematic approaches, ongoing education, and the right tools. Healthcare organizations that excel in medical billing accuracy implement structured processes that catch errors before claims submit. These best practices for medical coders, billing staff, and practice administrators create a foundation for financial success and regulatory compliance.
Let’s explore proven strategies that improve coding quality and reduce denial rates.

Leveraging Medical Coding Software and EHR Coding Integration
Modern medical coding software has revolutionized coding accuracy by incorporating intelligent edits, automated checks, and reference databases. These systems validate code selections in real-time, alerting coders to potential errors before claim submission.
Quality coding software includes built-in CPT and ICD-10 code databases that update automatically with annual changes. This eliminates the risk of using outdated codes.
Staying Current with Coding Updates and Guidelines
Continuing education is essential for maintaining coding proficiency. Both CPT and ICD-10 coding guidelines evolve annually, requiring coders to update their knowledge constantly. Professional medical coders dedicate significant time to learning new codes, revised guidelines, and changing payer requirements.
Professional certifications like CPC (Certified Professional Coder) and CCS (Certified Coding Specialist) from the AAPC require ongoing continuing education units (CEUs). These educational requirements ensure certified coders maintain current knowledge. Organizations should prioritize hiring and retaining certified coders who commit to professional development.
Official Coding References
These sites provide the codes and official guidelines from the organizations that create and maintain them.
- CPT Coding Resources – American Medical Association (AMA): The official source for Current Procedural Terminology (CPT) codes, guidelines, and related publications like CPT Assistant.
- ICD-10-CM – Centers for Disease Control and Prevention (CDC) / NCHS: Provides access to the ICD-10-CM (diagnosis codes) files, coding guidelines, and the official browser tool for the U.S.
- ICD-10/ICD-10-PCS – Centers for Medicare & Medicaid Services (CMS): Offers access to the official ICD-10-CM (diagnosis) and ICD-10-PCS (procedure) files and official guidelines for Medicare.
Professional Associations and Training
These organizations offer certification, continuing education, training programs, and industry resources for coders and billing professionals.
https://www.ahima.org/education-events/coding/
AAPC (American Academy of Professional Coders): The world’s largest organization providing medical coding, billing, and auditing training, certifications (like the CPC), and resources.
AHIMA (American Health Information Management Association): A leading association for health information professionals, offering certifications (like the CCA, CCS, and CCS-P) and extensive coding education.
Continuing Education for Medical Coders
Professional development opportunities abound for medical coders seeking to enhance their skills:
Professional certification programs provide comprehensive training and credential recognition. The AAPC offers certifications including CPC (Certified Professional Coder), CCS (Certified Coding Specialist), and specialty certifications in areas like cardiology or orthopedics. These programs include intensive training on coding guidelines, medical terminology, anatomy, and payer requirements.
Annual coding conferences bring together thousands of coding professionals for education and networking. HEALTHCON (hosted by AAPC) and AHIMA’s Assembly on Education feature sessions on coding updates, specialty coding issues, and emerging trends. These conferences provide CEUs required for certification maintenance.
Online coding courses offer flexible learning options for busy professionals. Many organizations provide webinars, on-demand courses, and virtual training covering specific coding topics. These range from basic medical coding basics for beginners to advanced specialty coding for experienced professionals.
Specialty coding workshops dive deep into complex areas like surgical coding, evaluation and management coding, or modifier usage. These intensive sessions help coders master challenging aspects of their specialty areas.
Conclusion: Mastering CPT vs ICD-10 for Billing Success
Understanding CPT vs ICD-10 is not just about memorizing codes—it’s about grasping how these two essential coding systems work together to document patient care, justify medical necessity, and secure proper reimbursement. CPT codes tell what medical services were performed, while ICD-10 codes explain why those services were necessary. Together, they create the complete clinical and financial picture that drives successful healthcare claims.
Remember these essential takeaways:
- Never submit a CPT code without a supporting ICD-10 diagnosis code
- Ensure your code pairings make clinical sense and meet medical necessity requirements
- Stay current with annual updates to both coding systems
Ready to eliminate coding errors and boost reimbursement rates? Explore our medical coding services and discover how expert support can transform your revenue cycle management. Our certified coding specialists ensure accurate code selection, proper documentation, and compliant claim submission—maximizing your reimbursements while minimizing denials. Need precise coding support for your practice? Contact us today for a consultation and let our expertise in charge entry and claim submission work for you.
What is the main difference between CPT vs ICD-10?
CPT codes describe what medical procedures and services were performed, while ICD-10 codes identify why those services were necessary by documenting the patient’s diagnosis or condition. Both are required for complete claim submission.
Can you submit a claim with only CPT codes or only ICD-10 codes?
No. Payers require both CPT vs ICD-10 codes on claims. The CPT code describes the service provided, and the ICD-10 code justifies medical necessity. Claims missing either code type will be denied.
Who maintains CPT vs ICD-10 codes?
The American Medical Association (AMA) owns and maintains CPT codes. The World Health Organization (WHO) maintains ICD-10 internationally, with the U.S. version (ICD-10-CM) adapted by the Centers for Disease Control and Prevention (CDC).
How often are CPT vs ICD-10 codes updated?
CPT codes update annually every January. ICD-10 codes update annually every October 1st. Healthcare organizations must implement these updates promptly to avoid claim denials for using outdated codes.
Do I need special training to use CPT vs ICD-10 codes?
Yes. Professional medical coding requires comprehensive training in anatomy, medical terminology, coding guidelines, and healthcare documentation. Professional certifications like CPC or CCS validate coding expertise and require continuing education to maintain.
